
By Stephanie Nguyen
About three years ago, five additional automated external defibrillators (AEDs) were installed on the outside of facilities within campus grounds. The school already had five of them, but they were kept indoors due to concerns about vandalism and theft. As AEDS became more commonplace, however, the school felt it became less of a concern.
“We discussed our needs with the district for our large campuses to make sure our community partners [that are] using our facilities had access to them as well,” head nurse Marci McLean-Crawford said. “We were granted five more devices and we mounted them all outdoors–that way they were not locked up and inaccessible.”
Around that same time, the Fountain Valley Fire Department gifted the school overdose kits that were placed next to all of the AEDs, which contain Narcan, an FDA approved brand of naloxone.
“Before we had those, we were putting the Narcan in with the AED, sticking it in that same container,” McLean-Crawford said.
AEDs are machines that deliver electrical shocks to a student or adult experiencing cardiac arrest. Unlike a heart attack, cardiac arrest requires immediate attention because the heart stops beating, and electric shocks could potentially revive the heartbeat. Naloxone, on the other hand, is a medication that can stop and reverse the effects of opioids, a category of drugs, by attaching to opioid receptors. Examples of opioids include heroin, morphine, codeine and fentanyl.
Currently, the school has ten AEDs. According to McLean-Crawford, they are now at the pool deck, athletic trainer, the football and baseball snack bars, the cafeteria, on the walls adjacent to the library’s entrance, outside the girl’s locker room facing the softball fields and near the 220 hallway. There are still a few of them that remain indoors, such as the ones in the health office and the gym.
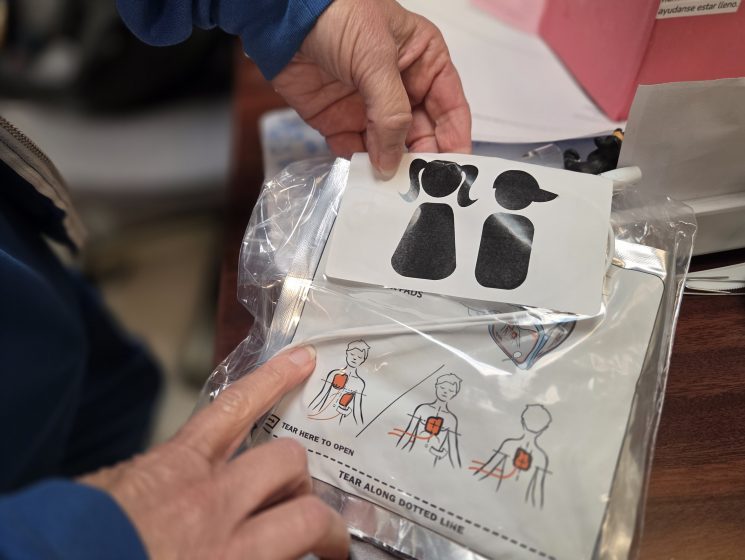
Inside the AED toolkit is the AED itself, the pads to administer the shock, a disc to do compressions on and audio instructions in both English and Spanish. However, there are staff on campus who are trained to do CPR.
“There’s an indicator on it that lets us know that it’s good and ready to go,” McLean-Crawford said. “So if [the indictator] was yellow or red, we wouldn’t be able to use it … it would mean that the battery was dead … Officer Hasegawa goes around to all the schools in the district and checks on these monthly, and will sign off that the battery is still good, that the pads are still good. If anything needs replacing, then he replaces it.”


And as for the overdose kits, they contain four milligrams of naloxone in single-use nasal sprays with usage instructions. Alongside the spray is a CPR mask and gloves.
“Because when you administer Narcan you also have to do CPR,” McLean-Crawford said. “You got to be able to do CPR to make that drug circulate and get it to move stuff off of the receptors.”
But what can be difficult is knowing when to administer aid. Some of the warning signs of cardiac arrest are pain in the shoulders, back, neck or chest, a shortness of breath, dizziness and nausea and/or palpitations. However, it can occur without warning, and a person may suddenly collapse and be unconscious without a pulse or breathing. The same can happen to someone experiencing an opioid overdose, but they may not feel any physical pain before the event.
“Usually they look blue or pale, [and] their pupils will be pinpoint, which means they’re constricted and really small,” McLean-Crawford said.
In case the symptoms were mistaken for either condition, neither the AED nor the spray will cause any negative effects. The AED can analyze a heartbeat and determine if an electric shock is needed and may advise not to deliver one if it isn’t necessary, and the naloxone would have no effect.
“It’s only made to bind with the opioids and to pull them off the receptors,” McLean-Crawford said. “But if there’s nothing there, then there’s nothing for it to bind to, and there’s no negative things that’ll happen because of it.”
Yet regardless of the situation, taking quick action can save a life; using either of these resources can give time for responders to arrive in the event of an emergency. She agreed that it doesn’t hurt to try to administer aid.
“Because you never know, and there’s nobody around to tell you,” McLean-Crawford said.





